What’s included?
- Introduction
- What is the neurobiological theory of addiction?
- What part of the brain causes addiction?
- How is the brain affected by substance abuse and addiction?
- Can brain changes caused by addiction be reversed?
- How can Delamere help with drug & alcohol addiction
Addiction is a brain disease. That’s what the NDA’s former director, Dr. Alan Leshner, proclaimed in his 1997 pivotal paper and countless others have supported this theory over the past quarter of a century. More recently, advancements in neuroscience and addiction research have continued to show that drug and alcohol addiction is less about how we behave and more about what’s going on deep inside our brains.
It makes sense if you think about. Why do people drink alcohol or take drugs? To alter their state of mind. To feel pleasure. To relax. To escape. To relieve pain. All actions and reactions that are ultimately controlled by the brain. And when we want to feel those sensations again, it’s the brain that triggers our cravings to repeat the behaviour. Over time, we almost become hard-wired to want more of a bad thing.
That’s a very simplistic way of describing what urges us to always want a cigarette after a meal or a glass of wine after a stressful day. But the science behind addiction – how it changes the way our brains think, feel and act – can really help us to understand the push and pull of substance abuse.

Need help for alcohol or drug addiction? Speak to Delamere
What is the neurobiological theory of addiction?
It sounds complicated, but neurobiology is essentially the study of cells in the nervous system and how they interact with each other. Imagine you forget to put oven gloves on and touch a hot oven. You instantly flinch and pull your hand away before even feeling any pain. Neurobiology explores how the brain helps you to make these conscious and unconscious decisions.
For years it was commonly believed that addiction was a choice or some sort of moral failing. This myth has now been debunked thanks to research into the neurology of the brain. Several studies have since shown that the development of addiction is directly related to changes in brain function and structure.
The cycle of addiction
It’s widely accepted that the cycle of addiction falls into three stages, each one having a different effect on the brain (1). When repeatedly exposed to substances over a long period, the brain alters its response to reward, stress and executive functions which creates sometimes irreversible changes. Damage that can affect the connections between neurotransmitter systems and different brain regions.
Binge/intoxication At this point, the person is enjoying drinking alcohol or taking drugs. The brain is engaging its pleasure receptors and dopamine levels increase. This results in feelings of euphoria, relaxation and intoxication.
Withdrawal/negative affect When a person stops using a substance, the brain’s reward pathways are impaired, and the stress response kicks in. The brain may respond in the form of convulsions, tremors, brain ‘zaps’, anxiety, paranoia and hallucinations.
Preoccupation/anticipation As the person starts to become preoccupied by the idea of drinking and taking drugs, the brain’s executive functions become compromised. This causes the brain to have difficulty regulating actions, emotions and impulses.
What part of the brain causes addiction?
There isn’t one particular brain part that is responsible for addiction. This complex organ has several regions and neurotransmitters that all work together. When drugs or alcohol are abused, these intricate parts get thrown out of balance. Different parts of the brain are disrupted at each stage of the addiction process and play a role in the onset of substance abuse as well as its development.
Top of the list is the mesolimbic dopamine system, or reward pathway of the brain. This key region is the part of the brain that gives us pleasure. Following years of substance abuse, the brain becomes desensitised to substances, such as opioids, cocaine and alcohol, resulting in increased dopamine release which can reinforce compulsive behaviour.
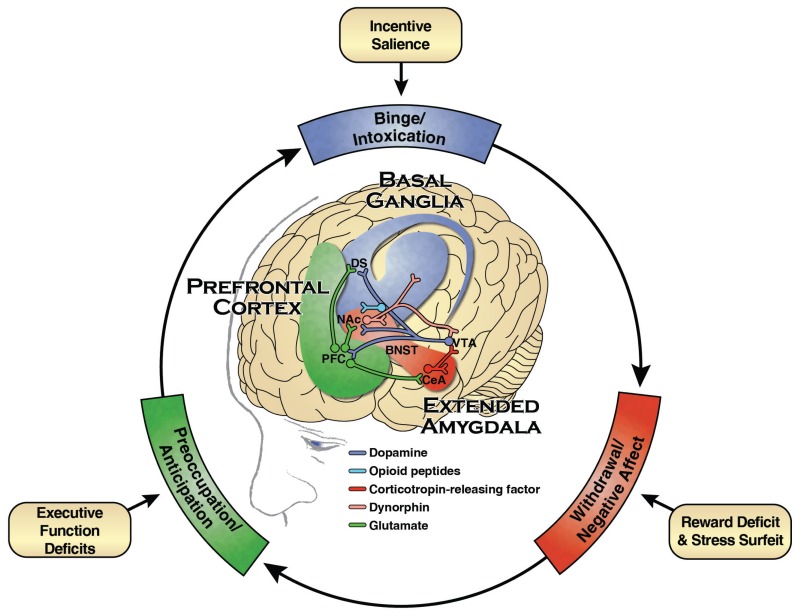
Within this network of brain structures, the amygdala plays a key role in reward, motivation and the processing of emotions. Interruptions in the regulation of stress hormones can increase anxiety and exaggerate a person’s response to stressful situations. Stress and anxiety are also common triggers for people struggling with substance abuse.
Usually, we can thank our pre-frontal cortex for helping us to make rational decisions, control impulses and regulate emotions. On the flip side, the addicted brain has structural damage that can lead to increased cravings, risk-taking and, ultimately, relapse.
Located near to the centre of the brain, the basal ganglia, is a group of structures that play a role in drug-seeking behaviour and habit formation. These interconnected brain regions are involved in controlling movement, reward, processing and learning. Damage to this region is the reason you might see an unsteady gait in long-suffering alcoholics.
These are just a few areas of the brain that are involved in addiction. The effects will be different for everybody. It’s important for psychologists and psychiatrists to understand how they interact with each other to ensure a person gets the most appropriate treatment.
How is the brain affected by substance abuse and addiction?
Several studies show that chronic drug addiction and alcohol addiction can cause a significant reduction in grey matter (2). Alcohol use disorder is associated with reduction in the size of the frontal lobe, which is the area that helps us with decision-making. Long-term cocaine and methamphetamine use is linked with reduced prefrontal cortex volume (3) and chronic opioid use can affect the regions of the brain that manage pain.
Other areas of the brain damaged by substance abuse include:
The cerebellum – Responsible for motor skills and balance, injury to the cerebellum can lead to difficulties walking, speaking and coordinating movement.
The hippocampus – As the region associated with memory and learning, years of substance abuse to the hippocampus can impact memory and the ability to learn new things.
Stress response – If the brain is stuck in a constant ‘fight or flight’ mode a person may be angry irritable, stressed, anxious or depressed.
Can brain changes caused by addiction be reversed?
When you repeatedly abuse any part of the body it eventually takes its toll. The good news is that some brain damage can be reversed, especially if treated quickly and effectively. It all depends on how much and how often you’ve been using, your family history and environmental factors.
Studies show the brain can recover from structural damage caused by addiction with abstinence, rehabilitation and lifestyle changes. There are also several medications that can help to rebalance brain chemistry. For instance, methadone, buprenorphine and naltrexone are all commonly prescribed as part of a residential rehab programme to manage withdrawal symptoms.
Other common approaches to restoring healthy brain function include Cognitive Behavioural Therapy (CBT), motivational interviewing and mindfulness techniques. These can all help the individual to address the cause of their addiction and develop healthier thought patterns.
Most problems can be managed with the right treatment and support. However, some people take longer to recover. Heavy alcohol use can lead to long-term issues that may require additional support. Post Acute Withdrawal Syndrome (PAWS) is a psychological condition where withdrawal symptoms last much longer than the initial detox period, sometimes for months or years.
If you’re worried about how alcohol or drug addiction is affecting your brain or you’ve noticed worrying changes in a loved one who is abusing, it’s important to seek professional help.
How Delamere can help with drug and alcohol addiction
At our purpose-built wellness retreat in Cheshire, we can treat both physiological and psychological brain changes that occur as a result of alcohol or drug addiction. Our residential rehab programmes are focused on getting you back to the best possible health through tailored medical support and intensive psychotherapy.

During your clinical detox, we can treat chemical imbalances in the brain with antidepressants and other medications. Once you are free from the reliance on substances we will help you understand the reasons behind your addiction with one-to-one counselling and group therapy sessions.
Cognitive Behaviour Therapy (CBT) is a proven talking therapy that can help to rewire the brain and retrain thinking to achieve desired behaviours. You can also access a wide range of somatic healing practices, from equine therapy to breathwork, which will guide you on the path to long-term recovery.
References
1. Uhl GR, Koob GF, Cable J. The neurobiology of addiction. Ann N Y Acad Sci. 2019 Sep;1451(1):5-28. doi: 10.1111/nyas.13989. Epub 2019 Jan 15. PMID: 30644552; PMCID: PMC6767400.
Pando-Naude, V., Toxto, S., Fernandez-Lozano, S. et al. Gray and white matter morphology in substance use disorders: a neuroimaging systematic review and meta-analysis. Transl Psychiatry 11, 29 (2021). Link here.
3. Ahmet O Ceceli et al. Common and distinct fronto-striatal volumetric changes in heroin and cocaine use disorders, Brai Brain, 2022, awac366. Link here.






